Hepatocellular carcinoma (HCC) remains a significant health challenge worldwide. Advances in diagnostic techniques, especially in Hepatocellular Carcinoma Ultrasound, are crucial. Dr. Emily Chen, a renowned expert in the field, states, “Ultrasound is essential for early detection of HCC.” This highlights the role of ultrasound in improving patient outcomes.
The evolution of Hepatocellular Carcinoma Ultrasound techniques is remarkable. New methods enhance sensitivity and specificity, but they still have limitations that require consideration. For instance, operator dependency can affect results. Ultrasound may miss small lesions, making comprehensive training vital.
Moreover, patient variability complicates interpretations. Different liver conditions can mask HCC signs. Despite these challenges, ongoing research aims to refine ultrasound technology. The insights expected in 2026 will likely address these limitations. Ultimately, the goal is to develop more effective diagnostic tools that provide clearer imaging and improve detection rates.
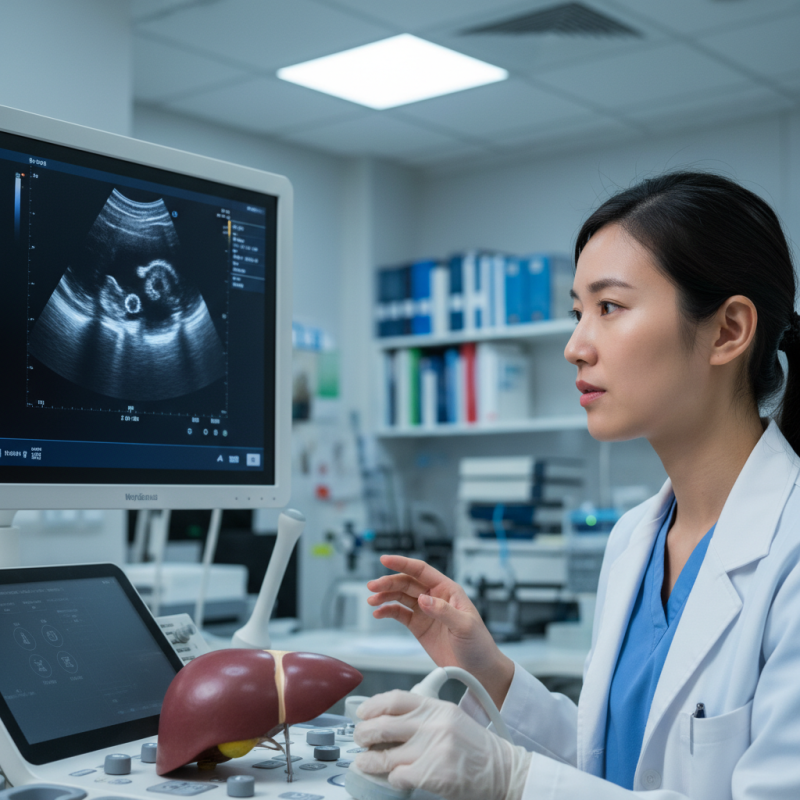
Hepatocellular carcinoma (HCC) is a major concern in oncology. It is one of the most common types of liver cancer. Recognizing the disease early can significantly improve patient outcomes. Ultrasound techniques are vital for early detection. They provide a non-invasive way to visualize liver abnormalities. Many healthcare providers use these methods as a first step in diagnosis.
Tips: When considering ultrasound for HCC screening, frequency is key. Regular check-ups can catch changes early. Also, be aware of the significance of the patient’s history. Chronic liver disease increases the risk of HCC. Patients with hepatitis or cirrhosis should be closely monitored.
Using ultrasound techniques effectively requires skill. Not all ultrasound equipment provides the same quality of images. Understanding the limitations of each method is crucial. It is important to assess potential false negatives. Techniques can vary greatly. Regular training is necessary for radiologists to stay updated. Awareness leads to better detection rates. This is an area where continuous improvement is essential. Each case presents unique challenges that researchers should address.
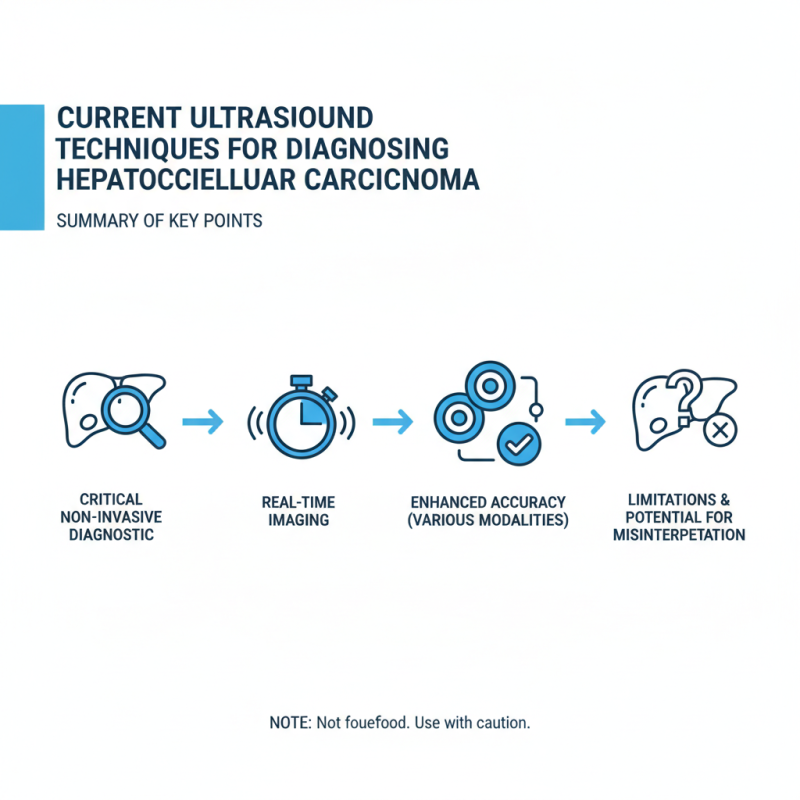
Ultrasound techniques are critical for diagnosing hepatocellular carcinoma (HCC). These non-invasive methods provide real-time imaging. They help identify and assess liver lesions effectively. Clinicians utilize different ultrasound modalities to enhance diagnostic accuracy. However, these techniques are not foolproof. They have limitations that can lead to misinterpretation.
One common technique is the use of contrast-enhanced ultrasound. This method employs microbubbles to improve visualization of liver lesions. While it often increases sensitivity, it can also result in false positives. Sonographers must be adept at distinguishing between benign and malignant lesions. Proper training is necessary to minimize errors.
Another approach is elastography, which measures liver stiffness. This technique is helpful in assessing liver fibrosis. However, it is less effective in detecting small tumors. The challenge lies in ensuring that small HCC cases do not go unnoticed. Ongoing refinement and research are essential in this field. As technology evolves, the hope is to improve diagnostics. Yet, the journey is filled with obstacles that require constant reevaluation.
The detection of hepatocellular carcinoma (HCC) has seen remarkable advancements with new ultrasound techniques. These techniques provide clearer images and better accuracy, greatly improving diagnosis. Enhanced resolution allows for detailed visualization of liver tissues. Clinicians can identify tumors earlier than ever before. This early detection is critical in improving patient outcomes.
Recent innovations include elastography, which measures liver stiffness. This method can indicate fibrosis progression, guiding further evaluation. Contrast-enhanced ultrasound is another breakthrough. It helps differentiate between benign and malignant lesions. However, these advanced techniques require specialized training. Not all medical institutions may have access to the latest technology, often limiting patient care.
While technology has improved, challenges remain. False positives can still occur, leading to unnecessary stress for patients. Not all cases are straightforward, and misinterpretation can happen. It’s essential to combine ultrasound findings with clinical judgment. Continuous education and awareness are vital for healthcare professionals. As imaging technology progresses, so must the strategies to keep pace with its implications.
Hepatocellular carcinoma (HCC) remains a leading cause of cancer-related deaths. Effective imaging techniques are crucial for early diagnosis and treatment. Ultrasound, CT, and MRI each have their strengths and weaknesses in detecting HCC.
Recent studies indicate that ultrasound can detect HCC with a sensitivity ranging from 65% to 95%. However, its accuracy heavily relies on the operator's skill and patient factors, such as obesity. In contrast, CT scans have a higher sensitivity, approximately 87%. Still, they expose patients to radiation. MRI, although costly, offers superior soft tissue contrast, making it invaluable for diagnosing small lesions.
In real-world applications, many clinicians face challenges when choosing the best imaging method. Each modality has limitations. Ultrasound is widely accessible but can miss early HCC. CT and MRI are more sensitive but may not be feasible in all situations. This variability underscores the importance of ongoing training for healthcare professionals. Integrating various imaging techniques might lead to improved outcomes for patients. Exploring these options allows for a more nuanced approach to HCC detection and management.
Innovations in ultrasound techniques for hepatocellular carcinoma (HCC) are rapidly evolving. Recent studies show that advanced imaging methods have improved the early detection rates significantly. Approximately 50% of HCC cases are diagnosed at advanced stages, limiting treatment options. However, using contrast-enhanced ultrasound (CEUS) has revolutionized this. It can differentiate malignant from benign lesions with over 90% accuracy.
Emerging technologies like elastography are enhancing our understanding of liver stiffness. This is vital for predicting HCC risk in cirrhotic patients. Data indicates that nearly 20% of cirrhosis patients develop HCC within five years. Integrating artificial intelligence (AI) into ultrasound readings also shows promise. AI can assist in interpreting complex images, making it easier for radiologists to detect abnormalities that may go unnoticed.
Despite advancements, challenges remain. Many ultrasound technicians lack training in advanced techniques, creating a knowledge gap. Access to high-quality imaging remains uneven across healthcare settings globally. Future research must address these shortcomings to ensure equitable care. A focus on education and resource allocation is crucial as we push forward in improving HCC outcomes through ultrasound methodologies.