Rehabilitation is a crucial aspect of recovery. Effective Rehabilitation Training Guidance can significantly enhance healing outcomes. Dr. Emily Carter, a renowned expert in rehabilitation, emphasizes, "The right guidance can make all the difference in a patient's recovery journey." This highlights the importance of expert strategies in rehabilitation.
Techniques for optimal recovery can vary widely. It’s essential to tailor rehabilitation programs to individual needs. One size does not fit all. Engaging with qualified professionals can lead to more personalized and effective approaches. Experts often note that recognizing each patient's unique circumstances is fundamental to their progress.
However, there are challenges in implementing these techniques. Not every practitioner follows the best practices. Patients may feel overwhelmed or unsure about their path. It’s vital to address these barriers. Encouraging open communication between patients and rehabilitation specialists can lead to better outcomes. Rehabilitation Training Guidance is not only about exercise; it's about building trust and understanding in the healing process.

In 2026, rehabilitation training techniques have evolved significantly. Innovative methods focus on individual needs, enhancing the recovery process. Recent studies show that personalized training can improve outcomes by up to 30%. These techniques consider mental and physical aspects of recovery. Balancing these elements is crucial for effective rehabilitation.
Evidence-based practices continue to emerge. A 2023 report highlighted that patients who engage in active recovery exercises exhibit a 25% faster return to daily activities. Techniques such as neuromuscular re-education and functional movement training play essential roles. They help restore strength and flexibility to injured areas, but not all patients respond the same way. Some may struggle with motivation or adaptability.
The integration of technology is another important trend. Wearable devices track progress, but the data can be overwhelming. Clinicians must interpret this information effectively. There’s a risk of relying too much on technology, which could undermine personal interaction. Practitioners are encouraged to blend high-tech approaches with empathetic, hands-on care for the best results.
Rehabilitation is essential for optimal recovery post-injury or surgery. Effective strategies use principles grounded in research. Studies show that individualized rehabilitation plans increase recovery rates by 30%. Personalized programs consider a patient's specific needs and goals.
Tips: Establish clear and achievable goals. Track progress regularly. Adjust plans as needed to stay on target.
Integrating strength training can significantly enhance recovery. A report by the Journal of Rehabilitation Medicine indicates that structured strength training programs improve functional outcomes by 25%. Focus on gradual increases in intensity to prevent setbacks.
Tips: Listen to your body. Avoid pushing through pain. Adapt the program to maintain engagement and motivation.
Effective communication between patients and healthcare providers is crucial. A comprehensive study published in the Archives of Physical Medicine and Rehabilitation highlights that collaborative care enhances patient satisfaction and adherence to rehabilitation plans. Make sure to voice concerns and ask questions throughout the process.
Tips: Keep an open line of communication with your therapist. Share feedback on what works and what does not.
Creating a personalized recovery plan is essential for effective rehabilitation. Every individual's needs differ based on their unique circumstances. Understanding this, clinicians must assess each person's physical and emotional state. A thorough evaluation can reveal strengths and weaknesses. This information is the foundation of a tailored recovery strategy.
Including specific goals is crucial. What does the individual want to achieve? Whether it’s improved mobility or reduced pain, goals should be realistic. Setting short-term milestones can encourage progress. These smaller achievements boost motivation and build confidence. Healing is not always linear. Some days will feel better than others. It’s important to reflect on setbacks without losing hope.
Incorporating feedback throughout the process can enhance outcomes. Regular check-ins allow for adjustments in the plan. This ensures the approach remains effective and relevant. Listen to the person’s experiences. Are they feeling overwhelmed? Adjustments might be needed to manage expectations. Personalization is an ongoing journey. The key is flexibility and responsiveness to changing needs.
| Technique | Description | Frequency | Duration | Targets |
|---|---|---|---|---|
| Manual Therapy | Hands-on techniques to improve mobility and reduce pain. | 3 times a week | 30 minutes | Musculoskeletal Issues |
| Aquatic Therapy | Exercises performed in water to reduce stress on joints. | 2 times a week | 45 minutes | Post-surgery Recovery |
| Strength Training | Resistance exercises to build muscle strength and enhance recovery. | 4 times a week | 60 minutes | Athletic Injury Recovery |
| Cognitive Behavioral Therapy | Psychological techniques to aid emotional recovery and coping strategies. | Weekly | 1 hour | Mental Health Recovery |
| Yoga | Mind-body practice to improve flexibility and reduce stress. | 3 times a week | 1 hour | General Well-being |
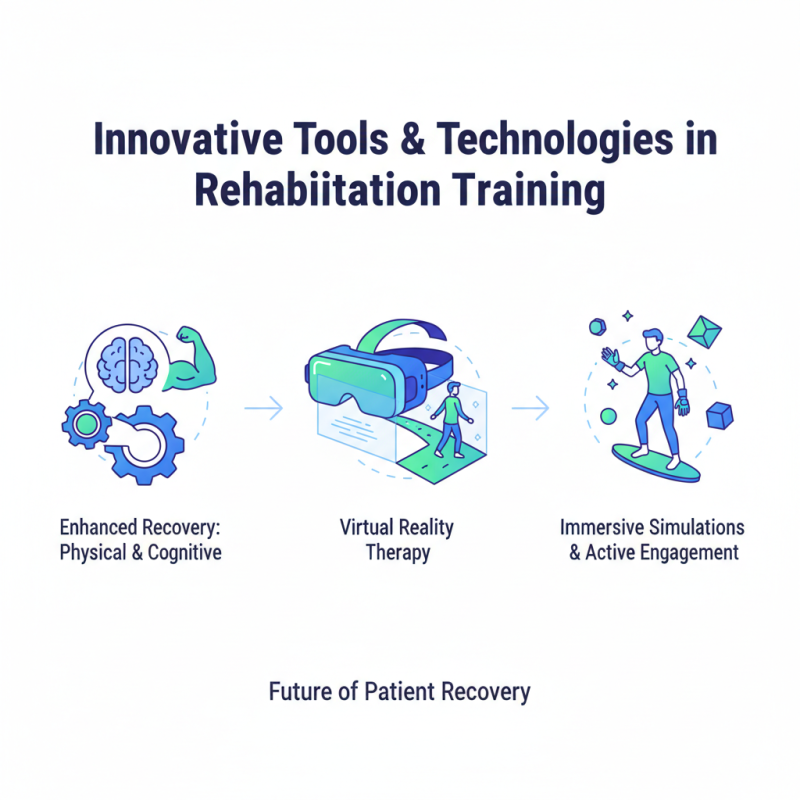
Rehabilitation training is rapidly evolving with innovative tools and technologies. These advancements enhance recovery experiences for patients. Virtual reality therapy is gaining traction. It provides immersive simulations that engage patients actively. This approach is useful for both physical and cognitive rehabilitation.
Wearable technology is another game changer. Smart devices track movements and monitor vital signs during exercises. This data allows therapists to tailor programs accurately. Patients can receive instant feedback. Yet, the reliance on technology can become a crutch. A balance between tech and traditional methods is essential.
Tele-rehabilitation is transforming how therapy is delivered. Remote sessions offer flexibility for patients, making rehabilitation accessible. However, not all patients may feel comfortable with online platforms. Personal connection is often lost in digital interactions. Therapists must adapt their strategies to maintain engagement in virtual settings. New tools bring promise, but careful implementation is crucial to maximize their effectiveness.
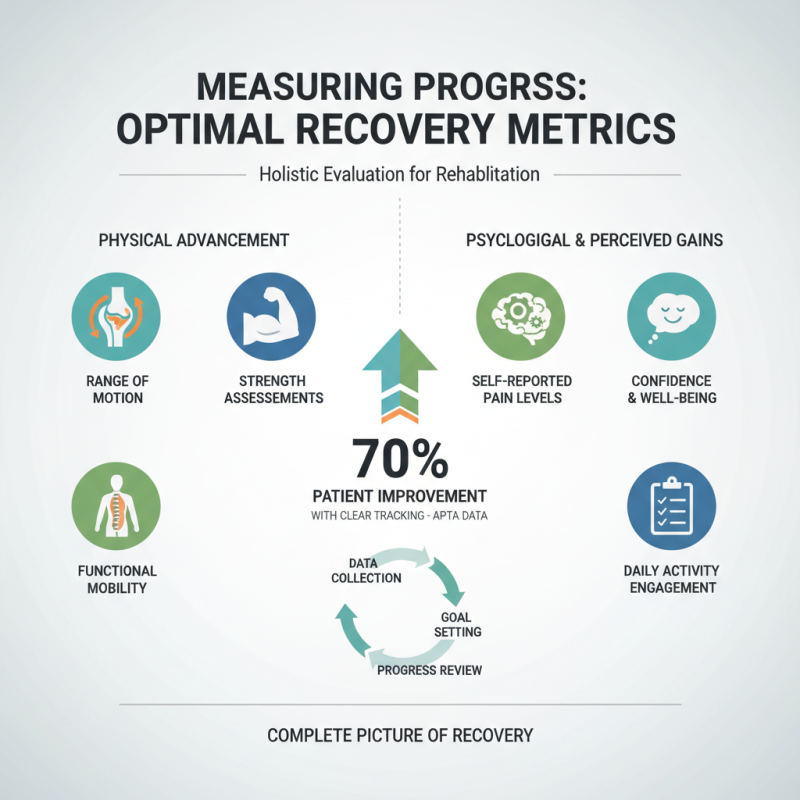
Measuring progress in rehabilitation is crucial for effective recovery. It's essential to establish metrics that reflect both physical and psychological advancements. According to the American Physical Therapy Association, nearly 70% of patients report improvements with clear progress tracking. These metrics can include range of motion, strength assessments, and self-reported pain levels. Each element plays a vital role in creating a complete picture of a patient’s recovery journey.
Tracking progress can be complex and sometimes leads to frustration. For instance, the variability in patient responses can complicate consistency. A study published in the Journal of Rehabilitation Research shows that 55% of patients may not see linear improvement. This emphasizes the importance of individualized assessments and the need to adjust rehabilitation techniques. Metrics must evolve as the patient progresses. Visual aids, like graphs, can help patients understand their journey. Yet, an over-reliance on numbers can create pressure or unrealistic expectations.
It's vital to remember that recovery isn’t just about data. Building a relationship with healthcare providers can enhance motivation. Emotional well-being is intertwined with physical recovery. Metrics should include self-evaluations of mood and motivation. This holistic approach ensures that all facets of recovery are monitored, making the rehabilitation process more effective and meaningful.