Rehabilitation Nursing Practice plays a crucial role in patient recovery. According to the American Nurses Association, effective rehabilitation leads to improved outcomes for millions of patients annually. However, challenges remain in delivering high-quality care. The need for specialized training and resources is evident. Experts believe that enhancing these practices can bridge this gap.
Dr. Sarah Johnson, a leading expert in Rehabilitation Nursing Practice, emphasizes, “We must prioritize continuous education to empower nurses.” This statement reflects the growing demand for well-trained rehabilitation nurses. Interestingly, statistics reveal that only 15% of nurses feel fully confident in their rehabilitation skills. This indicates an urgent need for improvement.
Modern healthcare systems should focus on establishing better training programs. Many nurses lack access to current rehabilitation strategies. Also, rising patient expectations can overwhelm staff. To address these issues, organizations must invest in ongoing education and resources. This is essential for elevating Rehabilitation Nursing Practice to meet today's healthcare demands.

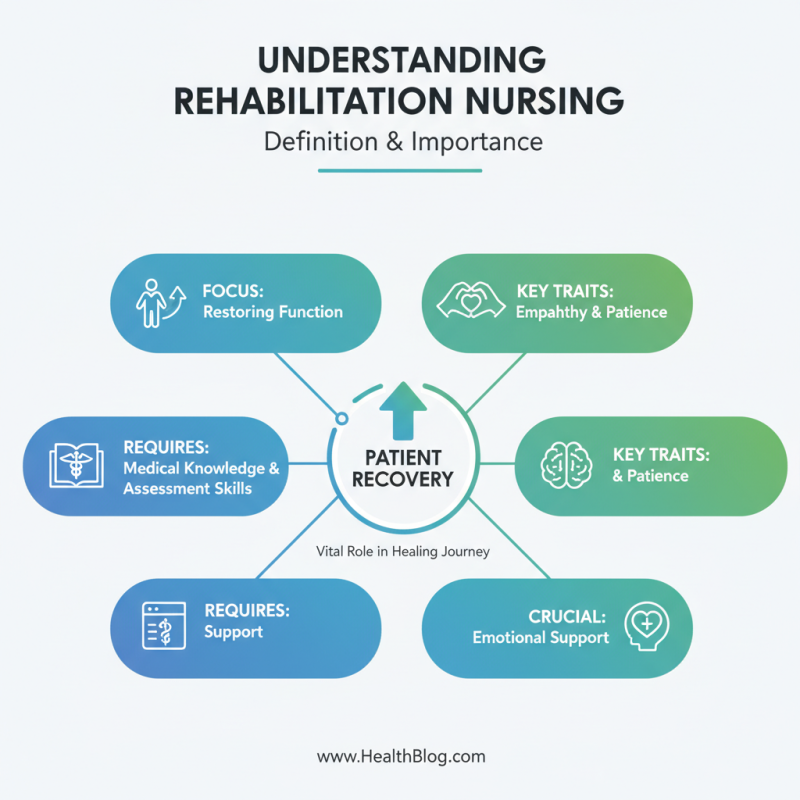
Rehabilitation nursing plays a vital role in patient recovery. It focuses on restoring functional abilities after illness or injury. This practice involves deep knowledge of various medical conditions. Nurses must be skilled in assessing each patient's unique needs. Empathy and patience are key traits for nurses in this field. Understanding the emotional aspects of recovery is equally important.
The significance of rehabilitation nursing cannot be overstated. It helps patients regain independence. Nurses often work closely with therapists and doctors. Collaboration is essential for creating personalized care plans. These plans address both physical and emotional challenges. There's always room for improvement in communication among care teams. Barriers can sometimes hinder effective collaboration. Nurses must advocate for their patients actively.
In practice, not all strategies will work for every patient. Resistance to rehabilitation occurs frequently. Some patients may not engage fully. This can leave nurses feeling frustrated. They must reflect on their approaches and adapt. Continuous education is crucial for staying updated. The evolving healthcare landscape calls for flexible practices. New strategies can lead to better patient outcomes.
Effective rehabilitation nursing practice is built on essential skills that support patient recovery. Communication is key. It involves listening and understanding patients’ needs. Nurses must ask open-ended questions. This helps to gather important information about the patients' experiences. Non-verbal cues, like body language, also play a significant role in conveying empathy.
Another critical skill is teamwork. Nurses often work alongside physical therapists, occupational therapists, and social workers. Collaboration enhances patient care. However, communication barriers can arise. These may lead to misunderstandings among team members. Regular meetings can help address these issues. Sharing insights keeps everyone aligned on patient goals.
Cultural competence is equally vital. Nurses should understand diverse backgrounds. Different cultures may affect how individuals respond to rehabilitation. This awareness helps in providing personalized care. However, it can be challenging to balance cultural sensitivity with clinical effectiveness. Continuous education and training can help nurses navigate these complexities in daily practice.
Evidence-based approaches are essential in rehabilitation nursing to improve patient outcomes. Research shows that patients who receive evidence-based care experience better mobility and increased independence. For example, interventions like task-oriented training can enhance functional recovery significantly. According to the Journal of Rehabilitation Research, using structured gait training programs leads to a 30% improvement in mobility for stroke patients.
Tips: Assess each patient's unique needs. Tailor the rehabilitation process based on their preferences and abilities.
Despite advancements, challenges remain. Some rehabilitation nurses may struggle with integrating new evidence into daily practice. A lack of continuous education can create barriers. Thus, providing regular training sessions is vital for fostering a culture of evidence-based practice.
Tips: Encourage team discussions about recent research. Create a platform for sharing successful case studies among staff.
Measurement tools can help evaluate the effectiveness of rehabilitation strategies. Tools like the Functional Independence Measure (FIM) and the Barthel Index assess patient progress quantitatively. Nurses often overlook these resources, limiting their ability to track improvements effectively. Regularly utilizing these tools can enhance care strategies, ultimately benefiting patients.
Collaboration with multidisciplinary teams is essential in rehabilitation nursing. It fosters a holistic approach, enhancing patient outcomes. Nurses must communicate effectively with physical therapists, occupational therapists, and social workers. Each professional brings unique insights, creating a well-rounded care plan.
Despite the benefits, challenges arise. Miscommunication can lead to fragmented care. Team members may have differing priorities, causing friction. These issues require regular meetings to ensure everyone is on the same page. It's vital for team members to understand each other's roles, which can be complex.
Building trust among team members is crucial. This trust allows for open dialogue and candid feedback. Reflection on past collaboration experiences can highlight areas for improvement. Identifying successful strategies can strengthen future teamwork. Continuous learning and adjustment are necessary for effective rehabilitation nursing practice.
Continuous professional development (CPD) is essential for rehabilitation nurses. This ongoing process helps them stay updated with the latest practices and techniques.
Nurses can attend workshops and seminars that focus on innovative rehabilitation methods. These events also provide opportunities to network with professionals in the field.
Moreover, online courses have become a valuable resource. They offer flexibility, allowing nurses to learn at their own pace. Engaging with online forums can also enhance knowledge. However, it's crucial to evaluate whether the sources used are credible. Not all information available online is accurate or relevant.
Reflection is key in this process. Nurses should identify areas where they can improve. Self-assessment can guide their development. Seeking feedback from peers can also highlight blind spots. Balancing daily responsibilities while engaging in CPD can be challenging. Nonetheless, dedicating time to professional growth is vital for providing the best patient care.